Solving the mystery of Sophie’s high blood pressure

Sophie Lawrence loves “Baby Shark.” Like many other toddlers, she listens to the popular children’s song on repeat, bopping her head and mimicking the accompanying hand gestures. “Something about it just really calms her when she’s upset,” says her mother, Samantha.
Indeed, Sophie was rocking out to “Baby Shark” during a recent appointment with Dr. Deborah Stein, co-director of the Midaortic Syndrome and Renovascular Hypertension Center at Boston Children’s Hospital. Now 16 months old, she’s been seeing Dr. Stein and her colleagues for most of her young life.

‘A really bad feeling’
Although Sophie appeared perfectly healthy at her first pediatrician appointment, her parents soon began to have some concerns. “She wasn’t latching anymore when she nursed, and her color changed,” Samantha remembers. “We started to have a really bad feeling.” Samantha and her husband, Jay, made another appointment with their pediatrician, who recommended they travel to Boston Children’s from their home in southeastern Massachusetts, “just to be safe.”
But once in Boston, what might have seemed like first-time parent jitters soon turned more serious. When clinicians found that Sophie’s heart function was poor, she was admitted to the cardiac intensive care unit (CICU). Soon, her blood pressure was “through the roof,” says Samantha. “We knew things were serious, but we didn’t know why.”

Solving a medical mystery
Sophie ended up spending two weeks between the CICU and the regular cardiac inpatient floor, as clinicians from specialties including nephrology, cardiology, genetics, and infectious diseases tried to solve the medical mystery behind her severe high blood pressure. Along with Dr. Stein, Sophie received care from Dr. Leslie Smoot and Dr. Paul Esteso in the Heart Center. The latter, a clinical fellow, “took the time to check in on us and fill us in whenever he could. He was really concerned, not just about Sophie, but about my husband and me as well,” says Samantha.
Testing eventually showed that she had renovascular hypertension, severely high blood pressure that results from decreased blood flow to the kidneys. In fact, imaging scans revealed that the blood vessels leading to Sophie’s left kidney were so narrow that that the organ was barely functional. “It was a lot to process, but everyone was very helpful,” says Samantha. “They took the time to describe the problem and inform us so we could make the best decisions for Sophie.”
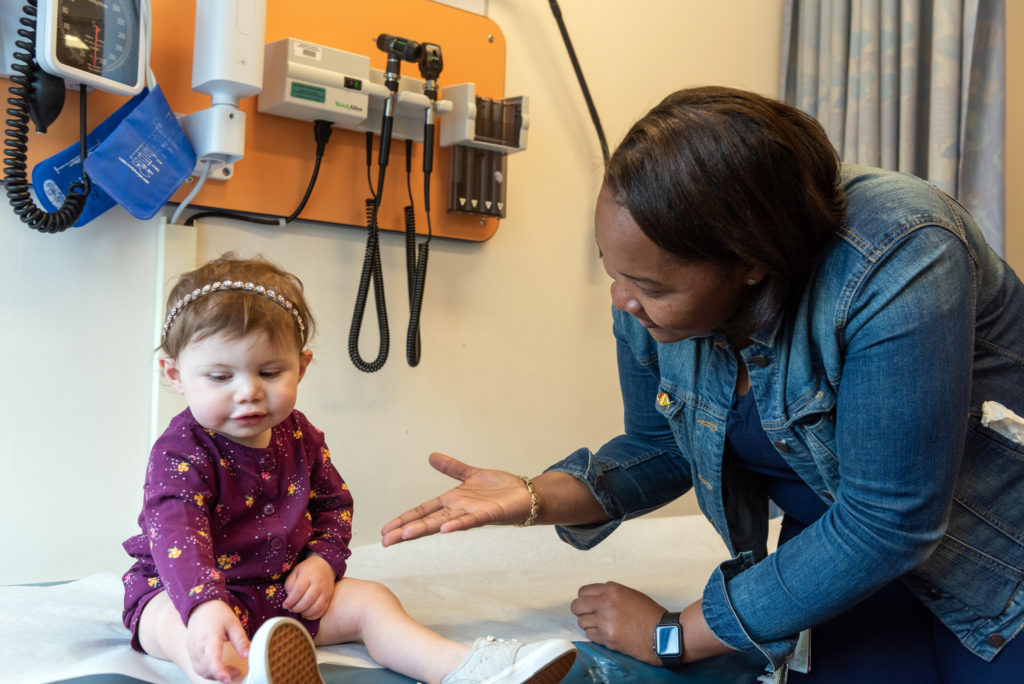
‘No place else we would go’
Those decisions included using medication prescribed by Dr. Stein to control Sophie’s blood pressure. She took the medication from the time she was diagnosed until January 2019, when the Lawrences were planning to take a trip to Grand Cayman. The family originally assumed they would need to stock up their daughter’s medication — which needed to be refrigerated — for their vacation. Instead, Dr. Stein suggested they try to slowly wean Sophie from the drug because she was doing so well. “She was so great about explaining our options,” says Samantha. “We trust her 100 percent.”
More than a year later, Sophie is completely off medication and thriving. When she’s not singing and dancing to “Baby Shark” or “Call Me Maybe,” she’s swimming, reading, and “throwing things like the remote control,” laughs her mom. A “huge daddy’s girl,” she also loves spending time with her grandmothers.
Although Sophie’s left kidney no longer functions, her right kidney is doing just fine, and her blood pressure is stable enough that she only requires checkups every four to six months. When she does return to the hospital, she’s excited to see Dr. Stein, as well as registered nurse Linda Pengeroth and program coordinator Jonette Jean-Louis. “We never thought our child would have a medical issue, but we couldn’t have picked a better place for her to receive care,” says Samantha. “There’s no place else we would go.”
Learn about the Midaortic Syndrome and Renovascular Hypertension Center.
Related Posts :
-

Not just another patient: Care for midaortic syndrome that’s ‘handcrafted’ for Iris
This past July, Iris Huot, her older sister, Audrey, and their parents, Jessica and Austin, gathered around their dining room ...
-

For Echo, treatment for midaortic syndrome was ‘MAGIC’
Most 7-year-olds don’t have high blood pressure, let alone blood pressure that hovers around 180/110 mm Hg. (“Normal” blood pressure ...
-

Maythum finally finds answers for midaortic syndrome
Maythum Mehdi was just 5 years old when he told his mother, Batul, that he was having trouble seeing: When he ...
-

Matt’s story: An innovative approach to midaortic syndrome
Until he was 12-and-a-half, Matt Sarracco had hardly missed a day of school. In fact, he had won awards for ...