I never thought this would happen to our son

On June 16, 2019, our 4-year-old son, Evan, fell off a jungle gym at daycare. At first, his daycare provider thought he was fine. He got right up and seemed to recover. She called me and we agreed to watch him to see if there were any changes.
A couple hours later, Evan started throwing up. As a pediatric physical therapist, I knew this was a bad sign. I raced to pick him up. The pediatrician urged me to head straight to Boston Children’s Hospital Emergency Department. I knew Evan had a concussion, and I was worried he might have bleeding in the brain. A CT scan showed Evan had a skull fracture and a subarachnoid bleed from his fall. But it also showed something much worse. Evan had a mass in a ventricle in his brain. This was devastating news. I had worked at Boston Children’s for 12 years, and I knew how bad this could be.
A devastating diagnosis: Brain tumor
After having an MRI, Evan was admitted to 9 North, the same floor where I had worked with so many children and teenagers with brain tumors. My husband and I were in shock, but were eager to find out what was wrong. The next morning Dr. Katie Fehnel came to meet with us. She confirmed what we’d seen in the scans — Evan had a mass in his left ventricle that could be a benign papilloma or a carcinoma.
Dr. Fehnel was so unbelievably kind and supportive in the way she shared this terrible news. She was straightforward and honest about what Evan was going to have to go through, but she also let me have my emotions and ask a million questions. She said what I as a parent needed to hear — that nothing I did or didn’t do during pregnancy or Evan’s life had caused this. There was no way to know how long he’d had the tumor. Finding it before it caused any problems, such as hydrocephalus, was huge for Evan’s prognosis.
Fixing Evan’s head
The plan was for Evan to go home for four to six weeks to allow his skull fracture to heal and then he would have surgery to remove the tumor. We went home and tried to be “normal” while this huge cloud hung over us. Evan recovered from his head injury and returned to the active life of a 4-year-old.
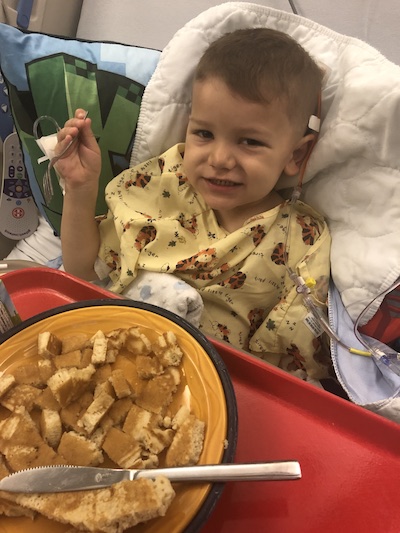
The morning of the surgery was the hardest of our lives. Evan was a champ though! He was all smiles through the pre-op process. Several of my former colleagues were waiting for us. Carrie Byrne, a child life specialist, filled Evan’s room with balloons and his favorite toys. In the operating room, Evan sat up, looked at everyone in scrubs and masks, and said, “Hi! Are you all going to fix my head?” He gave us a much needed laugh, and then quickly fell asleep.
Evan was in the operating room for the next eight hours. We were updated every 90 minutes by his operating room nurse, Jeanne Richard. She was fantastic, supportive, and hopeful. She gave us the confidence that our boy was being taken care of. Dr. Fehnel came out to speak with us after the surgery was complete. She was able to remove the entire tumor and was confident that Evan would not need a shunt to drain the ventricle.
Getting good news
The best news came on our last day in the hospital. Dr. Susan Chi, Evan’s oncologist, told us that Evan’s tumor was a grade 1 choroid plexus papilloma. No further treatment was needed other than monitoring. This was huge. Everything went as well as we could hope for. Moving forward Evan will be followed by Dana-Farber/Boston Children’s Brain Tumor Program. His first brain tumor clinic is coming up and we are eager to hear more good news.
Evan’s initial diagnosis was my worst nightmare. I’d worked with so many children diagnosed the same way. I never thought it would happen to my own child. But I’m grateful we live so close to the best hospital in the country for pediatric neurosurgery. I’m grateful to each and every person we came in contact with from pre-op to the Intensive Care Unit to 9N, neurosurgery, and oncology. Evan will get through this and go on to live a long and happy life, and I cannot thank Dana-Farber/Boston Children’s enough.
Learn more about Dana-Farber/Boston Children’s Brain Tumor Program.
Related Posts :
-

A new druggable cancer target: RNA-binding proteins on the cell surface
In 2021, research led by Ryan Flynn, MD, PhD, and his mentor, Nobel laureate Carolyn Bertozzi, PhD, opened a new chapter ...
-

Forecasting the future for childhood cancer survivors
Children are much more likely to survive cancer today than 50 years ago. Unfortunately, as adults, many of them develop cardiovascular ...
-

What orthopedic trauma surgeons wish more parents knew about lawnmower injuries
Summer is full of delights: lemonade, ice cream, and fresh-cut grass to name a few. Unfortunately, the warmer months can ...
-

Pediatric high-grade gliomas: Research reveals effective targeting with avapritinib
Pediatric high-grade gliomas, particularly H3K27M diffuse midline gliomas (DMG), are aggressive malignant brain tumors with a poor prognosis. ...





