When your baby has clubfoot: Answers for expecting parents
Treatment for clubfoot usually begins within a few weeks of a child’s birth. With prenatal ultrasound, parents often learn about clubfoot weeks or months before their child’s arrival.
Below, Dr. Collin May of the Lower Extremity Program in Boston Children’s Orthopedic Center answers questions about how meeting with an orthopedic specialist can ease expecting parents’ fears about a clubfoot diagnosis and their baby’s future.
What’s your goal when you meet parents who’ve recently learned their baby will be born with clubfoot?
Any abnormality on a prenatal ultrasound can be very scary. I’ve been through it myself. My child had a foot abnormality so I understand the feelings of shock, surprise, and fear many parents feel when they find out their baby has a clubfoot.
Our goal when we meet with parents is to reassure them that clubfoot is treatable. We tell them what the diagnosis means and what to expect from treatment and their child’s future mobility. Treating clubfoot is a long and involved process — parents need to understand and buy into that.
What question do you hear most often from expecting parents whose baby has clubfoot?
Parents’ most common question is “How will clubfoot affect our child’s mobility and function?”
Fortunately, we can tell them that with proper treatment, the vast majority of kids with clubfoot are able to run, jump, and play.

Clubfoot treatment starts after the child is born. Why does it help to meet with an orthopedic specialist before that?
It helps to establish a relationship with an orthopedic specialist early. A child’s birth is an emotional time. Having a rapport with the doctor who’s going to treat their child and having a plan can make delivering a child with clubfoot a lot less anxiety-provoking for parents.
What does clubfoot look like on an ultrasound?
Signs of clubfoot are a lot less obvious on an ultrasound than they are after the child is born. An obstetrician (OB) will suspect clubfoot if they see one or both feet in a certain position on the ultrasound (foot pointed downward and inward). Sometimes the foot may be positioned this way because there’s not much room in the uterus. If the foot is still in that position on subsequent ultrasounds, it is more likely the child has a true clubfoot.
How do expecting parents get referred to you?
Typically, if an OB sees an abnormality on a prenatal ultrasound, they reach out to the Maternal Fetal Care Center (MFCC). If a baby shows signs of clubfoot, the MFCC will refer the expecting parents to us.
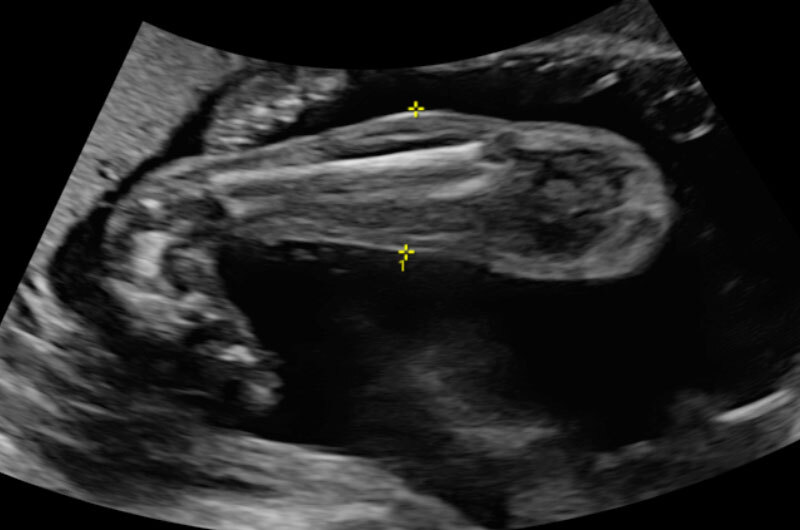
Do you ever think a child has a clubfoot on the ultrasound and find out when they are born that they don’t?
In general, if parents are referred to us for prenatal consultation, it’s likely their child has clubfoot. The ultrasound isn’t perfect though. There are times when we are fooled by the ultrasound appearance and a baby we thought might have a clubfoot turns out to be fine when they are born.
What questions should parents ask when looking for a provider to treat their baby’s clubfoot?
The most important thing to ask about is how much experience the provider has treating clubfoot. Treatment is labor intensive and needs to be done correctly. The physician needs to be knowledgeable enough to answer the parents’ questions, even after their child’s clubfoot is corrected. They also need to be able to recognize a possible reoccurrence and intervene before things regress too far.
How has the COVID-19 outbreak affected your patients with clubfoot?
At the start of the outbreak, we did not initiate any new treatments. But continuing treatment for children already in casts was considered an urgent need. We are now back to treating all of our patients with clubfoot.
What’s the most important thing you want parents to know about clubfoot?
Typical idiopathic clubfoot tends to be highly treatable. We can’t make clubfoot go away, but we can correct the foot into one that functions quite normally.
And while treatment takes a long time, it will not prevent a child from walking, running, or playing. By the time a child is ready to take their first steps, the casting phase will be over and the child will only need to wear the brace at night. By day, they can be a kid.
Learn more about the Lower Extremity Program.
Related Posts :
-

Diagnosed with clubfeet before he was born: Gabriel’s story
Cheryl Bratt and her wife, Sue, expected a routine visit when they went in for their 18-week ultrasound. Cheryl, a ...
-

A rare injury, a more determined player: Adrian’s knee dislocation
Adrian can barely remember a time when he didn’t play football. Now 16, he grew up watching games with his ...
-

How a meniscal transplant made me a Boston sports fan
I was in kindergarten when my knee started popping and cracking. My parents and I didn’t know it at ...
-

Hard and beautiful at the same time: Five lessons of raising a medically complex child
When they learned they were expecting a baby, Michelle and Stephen Strickland were delighted. The South Carolina couple looked forward ...





