Mary’s journey with genetic epilepsy

Lots of people don’t like the heat. It makes them feel uncomfortable and sluggish. But for Mary, being outside on a hot day means risking a seizure. So can running in gym class or having a fever. That’s because Mary has genetic epilepsy, a form of Dravet syndrome — a rare epilepsy syndrome caused by a genetic mutation — and a rise in her body temperature is a trigger for seizures.
Mary’s journey with genetic epilepsy began when she was just a baby. “When she was about 8 months old, she had a very long seizure and ended up in the intensive care unit (ICU) at Boston Children’s Hospital,” says Mary’s mom, Natasha. At that time, they couldn’t find the source of the problem, and because it was in the context of an illness and fever, diagnosed it as a febrile seizure and sent her home.
Fever is a first clue to diagnosis
But a few weeks later, Mary had another long seizure, again accompanied by a fever. “The repeated seizure with a fever combined with her age and the length of her seizures was a clue to the doctors that something else might be wrong,” says Natasha. It was then that the family was connected with Dr. Chellamani Harini in the Department of Neurology and Boston Children’s Epilepsy Center.
“I was insistent on finding the cause of Mary’s seizures, but Dr. Harini convinced us it was important to focus on controlling her seizures first, to minimize any long-term effects,” says Natasha. “They put her on medication to control her seizures, and we tried several until we finally found one that worked for Mary.”
Genetic test provides answers
With Mary’s seizures finally under control, they began searching for an answer to the cause of the problem. One of the medicines Mary had tried increased her seizures, and that, combined with a genetic test at age 2 1/2 provided the diagnosis: borderline Dravet syndrome. The genetic test found a change in the SCN1A gene, which can lead to many forms of epilepsy, including Dravet syndrome. In addition to causing many kinds of seizures, Dravet syndrome can also cause developmental delays and cognitive impairment.
“We had never heard of the condition, so when we looked it up on the internet and saw the words ‘rare,’ ‘catastrophic,’ and the course it could follow, we were very scared of where she would fall on the spectrum,” says Natasha.
Dr. Harini says that looking back, it was a miracle that the medications worked for Mary. “Many children with genetic epilepsies need to take several medicines and often still have continued seizures,” she says.
On track developmentally
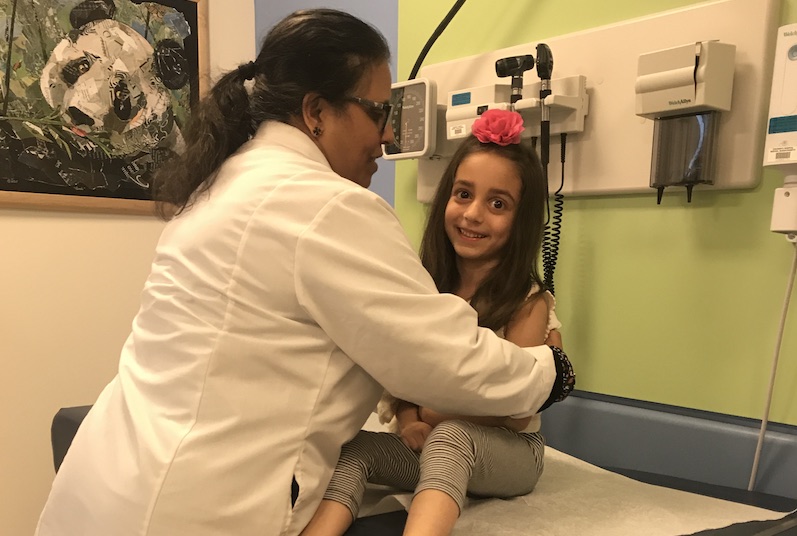
Fortunately, to date Mary has been on track developmentally. Natasha believes this is due in part to their working closely with Dr. Harini to address any problems right away and helping Mary by engaging occupational therapy and physical therapy. Today, Mary sees Dr. Harini every six months to check her medication and run labs. They are also vigilant about keeping her body temperature on an even keel.
“We check her body temperature and the room temperature several times,” says Natasha. “We do our best to prevent potential triggers, such as by keeping her home from school and not leaving the house on really hot days, and working with her teachers to have her sit when she’s doing too much during recess or gym class.”

An independent first grader in a regular classroom, Mary loves to run and climb, the very things that could cause her to heat up and induce a seizure,” says Natasha. “It always tugs at our heart strings when we have to tell her to slow down.”
Like many parents, Natasha says they may sometimes be a bit too overprotective. “Dr. Harini has really helped by encouraging us to allow Mary to live as normal a life as possible, and to allow her to be a child,” says Natasha.
Now 6, Mary is funny, passionate, bright, and loves to sing and make art. She also loves doing anything her 10-year-old brother, Gabriel, is doing. Gabriel faced his own health challenges as a young child — he was diagnosed with leukemia at age 3. Fortunately, Gabriel was successfully treated at Dana-Farber/Boston Children’s and has had no major health problems since.

Giving back to others
With the experience of having two children treated at Boston Children’s, Natasha wanted to give back and help other families. So, in June 2017, she joined the Family Advisory Council, and in November 2019, the newly-formed Neuroscience Family Advisory Council.
“When your kids are sick, the hospital is your only source of hope and the only thing you can really do is partner closely with them and hope that they will save your child,” she says. “For us it was a huge reassurance that our kids were seeing top doctors at the top Children’s Hospital, who not only provide excellent medical care, but also take that care to another level. It’s not just health care, but whole care. We are so grateful for the care our children received there.”
Learn more about the Epilepsy Center and the Epilepsy Genetics Program.
Related Posts :
-

“Princess June” reigns supreme over Rasmussen syndrome
What do you call a “girly” 5-year-old who adores dolls and frilly nightgowns? If you’re one of June Pelletier’...
-

The thalamus: A potential therapeutic target for neurodevelopmental disorders
Years ago, as a neurology resident, Chinfei Chen, MD, PhD, cared for a 20-year-old woman who had experienced a very ...
-

Could peripheral neuropathy be stopped before it starts?
An increase in high-fat, high-fructose foods in people’s diets has contributed to a dramatic increase in type 2 diabetes. This, ...
-

Status epilepticus: What’s changed, what to know, and a global perspective
Status epilepticus, or a prolonged seizure lasting more than five minutes, is a rare complication of epilepsy and a medical ...