Henry’s bladder exstrophy journey
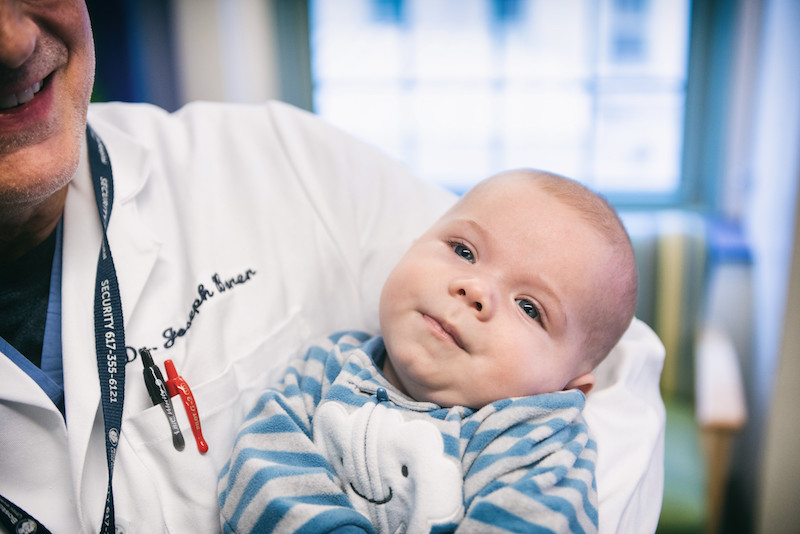
Just a few months into his young life, Henry Packer has traveled from the Netherlands to Utah to Massachusetts — and has gone from being a medical mystery to making a best friend with the same rare condition. It’s all part of his ongoing journey with bladder exstrophy, a congenital anomaly in which a baby’s bladder is formed both inside out and exposed on the outside of their body.

‘Full panic mode’
Henry’s parents, Tawni and Andrew, were living in Amsterdam with their three older children when he was born last fall. They were already prepared for a challenge: An ultrasound exam earlier in Tawni’s pregnancy led clinicians to believe that Henry would be intersex, a belief they held until the day of his birth.
But as the Packers welcomed their new son into the world, Andrew noticed that “something was off,” says Tawni. With only a midwife at their side — standard practice in Dutch health care — the couple went into “full panic mode.” Physicians at the hospital were stymied and sent photos of Henry to the country’s only pediatric urologist, hopeful for some insight.

The search for a surgeon
The next day, the Packers traveled by ambulance to meet that specialist, who diagnosed Henry with bladder exstrophy and explained that surgery would be necessary. But they found themselves hesitant to proceed. “He was a great doctor, but he had only performed about 20 repairs because many cases of bladder exstrophy are terminated before birth in Europe,” remembers Tawni. “We were nervous.”
A few weeks later, Tawni and Andrew reached out to Dr. Andrew Schaeffer, a pediatric urologist in their home state of Utah, who gave them the names of some top surgeons to contact. These included Dr. Joseph Borer, director of the Bladder Exstrophy Program at Boston Children’s Hospital, where Dr. Schaeffer had trained. “He told us that Dr. Borer had treated hundreds of kids with bladder exstrophy,” says Tawni.

Seeing patients as people
Although the Packers spoke with other physicians in their search, they say that they immediately felt comfortable during their first call with Dr. Borer, nurse practitioner Lauren Cullen, and registered nurse Rosemary Grant. “They spent an hour and a half talking with us,” says Tawni. In fact, she says, the first question that Dr. Borer asked was what her baby’s name was. “He just really cares about Henry and sees him as a person, not a condition,” she says. What’s more, Dr. Borer explained that most babies born with bladder exstrophy are otherwise very healthy and that Henry’s bladder was the only organ that had formed abnormally.
After a few more phone conversations, Henry and his parents were on their way to Boston. On October 7, he underwent the 14-hour surgical repair. “It was daunting,” Tawni admits. But as Henry recuperated, Dr. Borer was by his side, even checking in on him during his days off and weekends.

Moving forward
Now 5 months old, Henry is a happy, smiling baby who’s obsessed with his favorite toy, a frog named Freddie that makes him laugh and accompanies him everywhere. And he has another new buddy, too. While Henry was recovering from surgery, he met Stetson, another baby with bladder exstrophy who had also just been treated by Dr. Borer. The families have become close and plan to stay in touch.
The Packers have returned to the U.S. from the Netherlands, primarily for access to specialized care, and live in Utah. And Henry is thriving: His bladder and bones — which can become weakened as a result of bladder exstrophy — are healing well. Although, like most kids with bladder exstrophy, he’ll likely need additional procedures as he gets older, the future looks bright. “He’s doing great and hasn’t had any setbacks,” says Tawni. “He just keeps moving forward.”
Learn about the Bladder Exstrophy Program and read Stetson’s story.
Related Posts :
-

Machine learning algorithm could offer urologists a “crystal ball” for predicting VUR
Hydronephrosis is a common congenital anomaly that’s increasingly identified during prenatal ultrasound. Although ultrasound is also the first-line test ...
-

One day closer: Second opinion for urologic pain changes Iker’s life at last
Like many kids, Iker Guzman enjoys playing with LEGO toys. But there was nothing lighthearted about the day a few ...
-

It takes a village and the world: Tariq’s care for Tourette syndrome
When your child is sick but you can’t figure out the cause or how to fix it, it can ...
-

Care for a prince: One family’s inspiring journey for encephalocele repair
To hear Peter and Eunice of Kenya tell the story of their son, Prince, is to hear about the power ...