Mia’s team: Working together to address aspiration

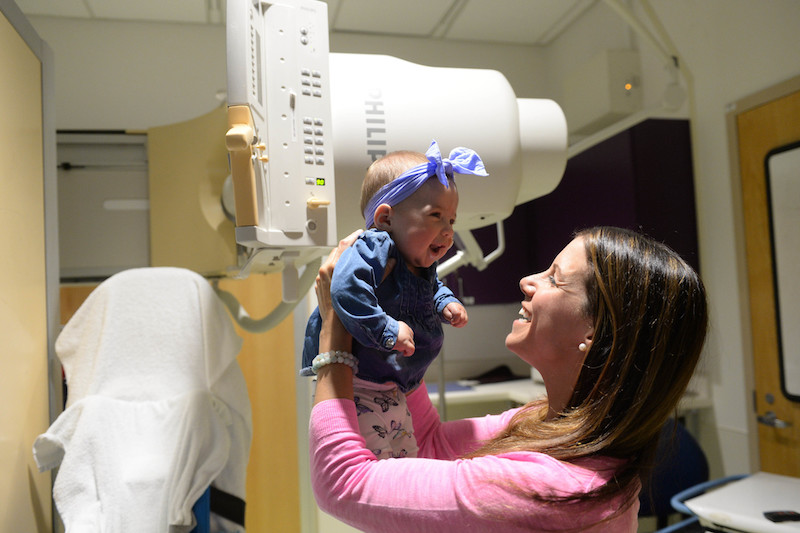
Seven-month-old Mia Petrelli sits in a chair in the darkened room. As Kara Larson, a speech language pathologist in the Aerodigestive Center at Boston Children’s Hospital, spoons different foods mixed with liquid barium into the little girl’s mouth, a nearby video screen displays real-time images of her anatomy. It’s part of a modified barium swallow study, a test designed to evaluate a child’s ability to safely eat and swallow. At times, her parents join in feeding her, too. “We know there’s a long road ahead,” says her mother, Maria. “But we’re all here to help Mia.”

A forgotten skill
Although Mia was born prematurely, she initially appeared healthy. “Everything seemed fine in the beginning,” her father, Bob, remembers. “She was breathing on her own and doing great with feeding — but then it all just slowed down.” A precautionary ultrasound raised an alarm: The ventricles in Mia’s brain were enlarged, which can be a sign of hydrocephalus. Fortunately, a wait-and-see approach paid off, and the problem resolved on its own.
Yet Mia was now dealing with a different difficulty. A swallow study revealed that she was aspirating every time she tried to feed, causing liquid to enter her lungs. Because of this, she had to take a break from bottle feeding for a couple of months. She was allowed to practice a small amount every day, but doing it so infrequently caused her to develop an aversion to the bottle — and she started to retch and spit up when it entered her mouth. “It was really discouraging,” says Bob. “It was like she had forgotten how to do what she had started out doing so well.”
Managing expectations
The next few months were filled with ups and downs. Mia came home with a nasogastric (NG) tube, which delivers nutrition to her stomach via a tube through her nose. It isn’t always simple to manage: As she’s grown and gotten stronger, she’s been able to pull out her NG tube, requiring ongoing monitoring and frequent replacements.
Encouraging Mia to try eating on her own hasn’t been easy, either. For months, the Petrellis tried rubbing applesauce or other pureed food on her lips, hoping she would taste it. If it went too far into her mouth, she would often gag or vomit. “When she opens up her mouth to taste food, we get excited she’s about to have everything ‘click,’ but we’re slowly learning that it doesn’t always work that way,” says Maria. “We’re realizing that we need to manage our own expectations.”
It’s an understandably challenging situation for any couple. “It can be stressful,” admits Bob. “We let each other have our frustrations in the moment and then we squash it. We work together as a team for Mia.”

‘We got really lucky’
Also on that team: Larson, registered dietitian Tracie Clarke, nurse practitioner Zoe Chin, and Dr. Daniel Duncan, who help ensure that Mia receives regular feeding and swallowing therapy, nutritional guidance, and the care she needs to thrive. “They’re the experts, but they respect us as parents,” says Maria. “We really appreciate that.”
And the Petrellis have found that being first-time parents has its benefits when dealing with a chronic medical concern. “She’s our only child, so this seems normal to us now,” explains Bob. “And Mia doesn’t know anything else, so it’s normal for her, too.”
Despite her feeding difficulties, Mia is a good-natured, snuggly, sweet little girl who loves to smile. “She hardly ever cries and almost always sleeps through the night,” says Maria. “We actually got really lucky.”
Learn about the Aerodigestive Center.
Related Posts :
-

An unbreakable bond: Brothers turn medical complexities into superpowers
“Look! Is that one JetBlue? I think that one’s Delta!” Running through the grass, climbing on the jungle gym, ...
-

From swallowing troubles to doughnuts: How vascular ring treatment helped Everly
By the time she was a year old, Everly Parisee was frequently wheezing. Then she had trouble swallowing foods. Her ...
-

New insight into the effects of PPIs in children
Proton-pump inhibitors (PPIs) are frequently prescribed to suppress stomach acid in patients with gastroesophageal reflux disease (GERD). Prescribing rates of ...
-

How transnasal endoscopy got Jamie back on the golf course
Jamie is like most 15-year-olds — he goes to school, hangs out with his friends, and still makes time to get ...





